Overview
what it is and why it matters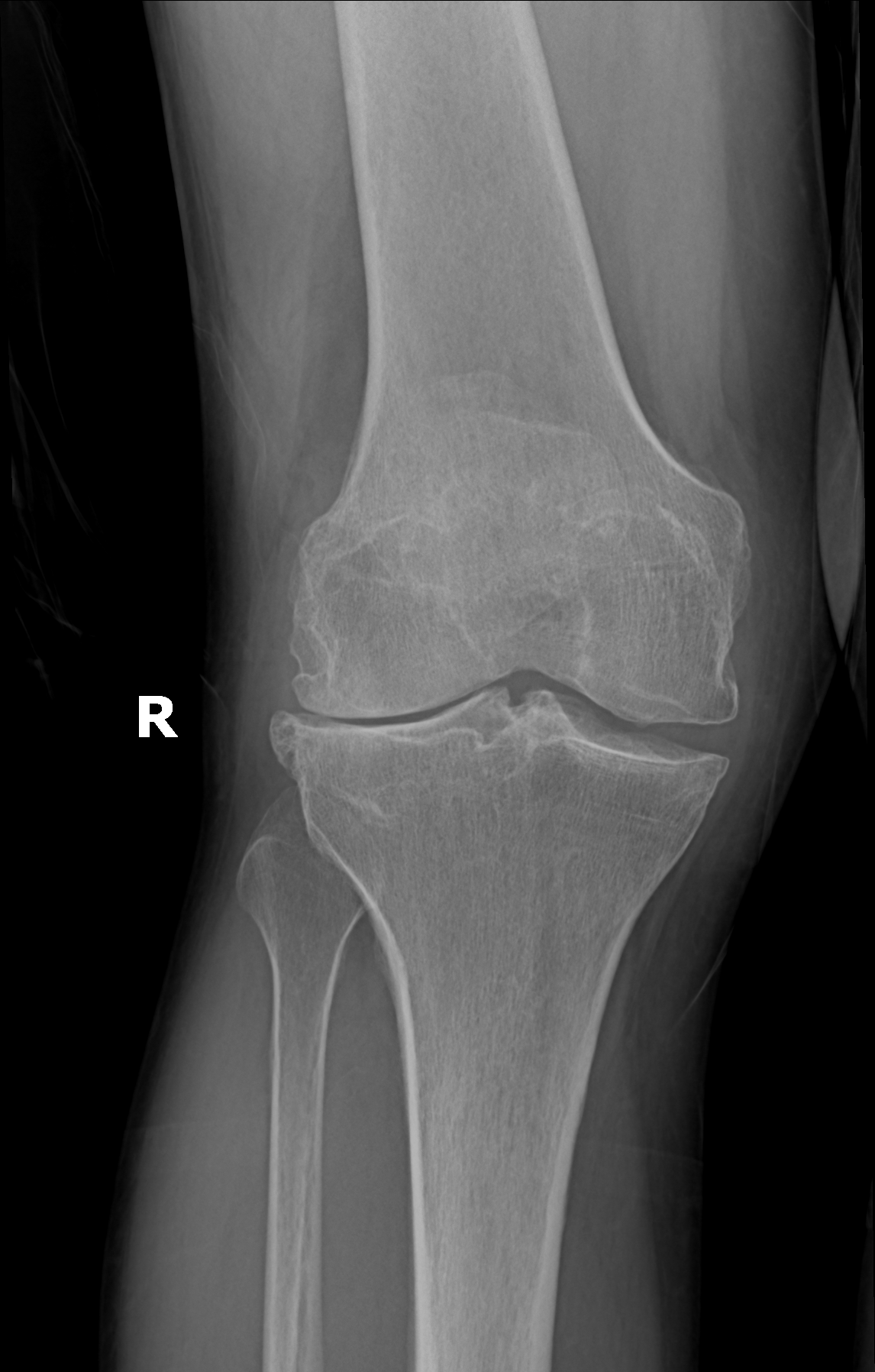
Knee osteoarthritis is the slow wearing-out of the smooth cartilage that lines the three compartments of your knee — the inner side (the medial compartment), the outer side (the lateral compartment), and the joint behind the kneecap (the patellofemoral compartment). Cartilage itself has no nerves, which is why a worn knee can look bad on X-ray years before it starts to hurt. The pain comes from the bone underneath the cartilage (the subchondral bone), which is richly innervated. As the cushion thins past a critical point, the bones start to contact each other directly, the joint lining (the synovium) gets inflamed and thickens, and the body lays down small bony outcroppings at the rim of the joint (called osteophytes) trying to stabilize what's becoming unstable. The practical result is the deep, achy pain patients describe as worse on stairs, worse after sitting, and worse at the end of the day.
Most knee arthritis is what we call primary — the cumulative result of decades of normal use, your genetics, and your body weight. Secondary arthritis is when there's a specific earlier event you can point to: a meniscus tear, an ACL rupture, a fracture that ran into the joint surface, or a leg whose alignment loads one side more than the other — a bowed leg (varus) wears the inner side first; a knock-kneed leg (valgus) wears the outer side first. Body weight matters across all of these: every pound translates to three or four pounds of force across the knee with each step, which is why weight management has such a direct effect on cartilage health.
Anatomy & Mechanism
why the knee wearsThe knee joint carries 3 to 4 times your body weight during level walking, and up to 6 times body weight going up stairs. Cartilage spreads that load evenly; the meniscus cushions add shock absorption. When cartilage thins, the load concentrates on smaller areas of bone, the joint becomes inflamed, and the body lays down bone spurs trying to stabilize itself. Because the inner side of most knees takes more load than the outer side, it wears out first — which is why many people with knee arthritis gradually become more bow-legged over time. Losing the meniscus (from a tear, or from a previous meniscus surgery) speeds up the cartilage loss on that side.
Three compartments of the knee
Symptoms
what patients describeThe pain pattern is recognizable. It's a deep ache rather than a sharp pain. Most patients have what we call the gel phenomenon — the knee gets stiff after sitting still for a while and takes a few minutes of walking to loosen back up. Morning stiffness usually lasts under 30 minutes, distinct from the longer morning stiffness of inflammatory arthritis. Stairs (especially going down) hurt more than level walking. The pain builds through the day and is at its worst by evening. Many patients hear the joint grinding or feel a catch as the worn surfaces meet, especially when a degenerative meniscus tear coexists. Recurrent swelling and a sense of warmth around the joint after activity are common.
As the disease advances, the knee starts to look different — a bowed leg or a knock-kneed leg as one compartment wears faster than the other. Swelling becomes a near-constant feature rather than something that comes and goes. Night pain that wakes you up and the loss of deep flexion (difficulty kneeling, squatting, or sitting cross-legged) are the late signals — when these show up, surgery is usually on the horizon.
Diagnosis
exam first, imaging secondWeight-bearing X-rays are the imaging standard — a standing anteroposterior, a lateral, and a patellofemoral view (sunrise or Merchant). Non-weight-bearing films routinely underestimate joint-space narrowing because the cartilage is not being compressed by body weight. Radiographic severity is graded on the Kellgren-Lawrence scale (0—4).
MRI is not required to diagnose OA and is reserved for targeted questions — a mechanical meniscus tear in a younger patient, suspicion of osteonecrosis, or soft-tissue pathology that would not show on radiograph. Laboratory testing is limited to cases where inflammatory or crystalline disease is suspected.
Medial cartilage loss vs. intact lateral compartment
Nonoperative Treatment
first line for most patientsThe first goal of treatment is to make the joint comfortable enough to keep using it. Most patients improve meaningfully with a combination of weight management, strengthening, and staged pain control — no injection, no surgery required.
Weight management & low-impact conditioning
Every pound lost takes roughly three to four pounds of load off each knee. Cycling, swimming, and elliptical work preserve cardiovascular fitness without concentrating force on the joint.
Physical therapy
Strong quadriceps — especially the inner portion that attaches near the kneecap — act as a shock absorber at heel strike and reduce the force the cartilage has to absorb. Hip and core strengthening round out the program.
Oral and topical analgesics
Anti-inflammatory medications (ibuprofen, naproxen, meloxicam) provide meaningful pain relief when used intermittently and when heart, stomach, and kidney health allow. Topical diclofenac applied to the skin over the knee is a good alternative when oral anti-inflammatories are not a safe option.
Cortisone injection
An intra-articular corticosteroid injection provides meaningful relief in the right patient and is useful as a bridge to therapy gains or a planned surgery. Repeated frequent injections are avoided.
Hyaluronic acid (viscosupplementation)
Hyaluronic acid is a lubricating fluid injection and has its strongest evidence in the knee. It is a reasonable option for patients who want to delay a knee replacement.
Unloader bracing
An unloader brace uses a three-point bending mechanism to redirect force away from the worn compartment. Patient selection matters — it works best when only the medial or only the lateral side is arthritic and the ligaments are intact.
Biologic injections (PRP)
Platelet-rich plasma is prepared from your own blood and injected into the joint. It has shown promise in mild-to-moderate osteoarthritis and is considered after standard options have been tried. PRP is not covered by insurance and is offered at a flat self-pay rate.
Operative Treatment
when function no longer respondsThe decision to operate is rarely driven by the X-ray alone — it rests on how much the knee is interfering with life. Surgery is considered when nonoperative care no longer provides adequate relief, when pain is waking you at night, when activities that matter are being avoided, or when daily pain medication has become necessary to function. Modern total knee replacement is one of the most successful operations in medicine, with more than 95% of implants still in place and working well a decade after surgery.
Primary procedure
Total knee replacement
Resurfacing of all three knee compartments. The standard operation for end-stage tricompartmental or advanced bicompartmental disease.
Learn about this procedure →Additional option
Partial knee replacement
For isolated medial or lateral compartment disease with intact ligaments — resurfaces only the worn compartment, preserves native anatomy, and offers a faster recovery.
Learn about this procedure →Additional option
High tibial osteotomy
Realignment procedure that unloads the worn compartment in younger, active patients with varus malalignment and unicompartmental disease.
Learn about this procedure →Recovery & Expectations
what care looks like after surgeryRecovery after knee replacement moves through predictable phases, but the pace is individual. Early rehabilitation focuses on swelling control, quadriceps activation, and restoring range of motion. Strengthening progresses as healing permits, and walking distance and gait quality become the benchmarks for weaning any assistive device. The final phase is a gradual return to everyday activity and low-impact recreation.
Driving, desk work, and physical labor resume when your OSI provider confirms you are ready — based on motion, strength, and how the knee tolerates load, not on a fixed calendar. Venous thromboembolism prophylaxis is standard. Numbness along the incision is common early on and usually fades over time.
When to Contact Us
making the callSchedule an evaluation for knee pain that has persisted beyond six weeks, limits walking or stairs, wakes you at night, or no longer responds to over-the-counter medication. Call sooner for a locked knee, sudden inability to bear weight, fever with joint pain, or a painful swollen joint after trauma.
Providers Who Treat Knee Osteoarthritis
joint-replacement teamFurther Reading
authoritative sourcesExternal patient-education references and related OSI pages for additional background:




